Seborrheic Dermatitis and Dandruff
In vitro testing Microbiology powered
Dandruff and Seborrheic Dermatitis exist on a continuous clinical spectrum. While dandruff is considered the mild, non-inflammatory version localized to the scalp, Seborrheic Dermatitis is a chronic inflammatory condition that can affect the face, chest, and body.
The development of Seborrheic Dermatitis/Dandruff is driven by a complex interaction between the host's skin, oils, and microorganisms.
- Microbial Overgrowth (Malassezia): These lipophilic (oil-loving) yeasts are part of normal skin flora but over-proliferate in affected individuals. They produce lipases that break down skin oils (sebum).
- Lipid Metabolites (Oleic Acid): The breakdown of sebum releases free fatty acids, particularly oleic acid. In susceptible individuals, this acid penetrates the skin barrier, acting as a primary irritant.
- Host Immune Response: The immune system overreacts to these metabolites, triggering an inflammatory cascade (Th17/Th22 pathways). This causes the skin to speed up cell production, leading to the rapid shedding of "immature" skin cells that clump together as visible flakes.
These conditions result from a state of dysbiosis an imbalance in the complex ecosystem of fungi and bacteria on the skin surface.
Background of Seborrheic Dermatitis and Dandruff model
The Central Role of Malassezia (The Mycobiome)
The most significant microbial player is the genus Malassezia, specifically M. restricta and M. globosa. These yeasts are normal residents of human skin, but in Seborrheic Dermatitis and dandruff, they interact abnormally with the host.
The Bacterial Shift (The Bacteriome)
Recent high-throughput sequencing has revealed that dandruff and Seborrheic Dermatitis are not just about fungi; the bacterial community also shifts significantly:
- In healthy scalps, Cutibacterium acnes typically dominates.
- In dandruff and Seborrheic Dermatitis, there is a marked increase in Staphylococcus species (particularly S. epidermidis and S. capitis)
Vibiosphen can provide support for the microbiota characterization of clinical samples
Conventional microbiology or molecular approaches. Targeted or global approaches.
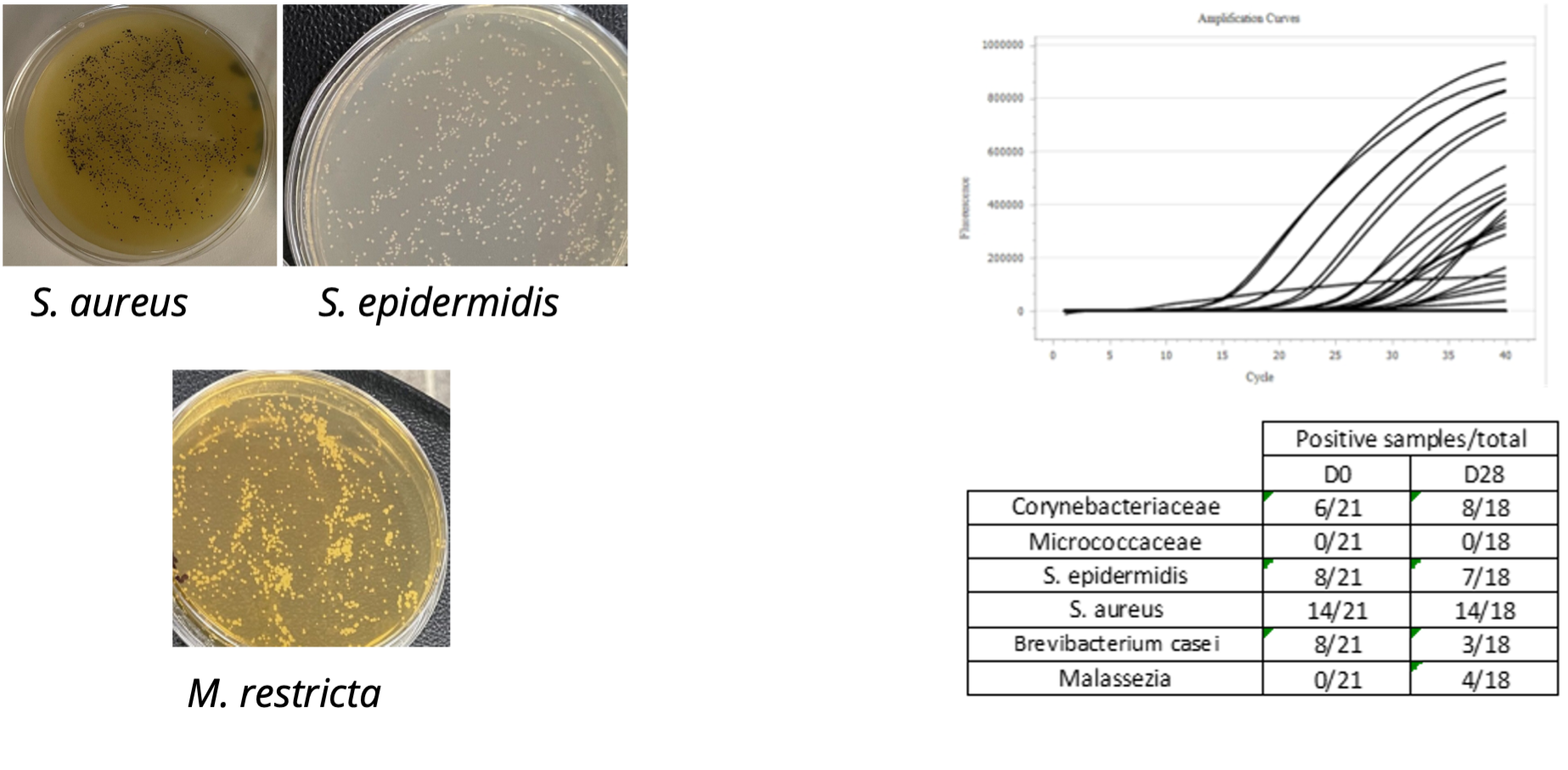
Vibiosphen has developed a scalp microbiome model (3 species) and a skin microbiome model (5 species) for screening compounds/therapeutics:
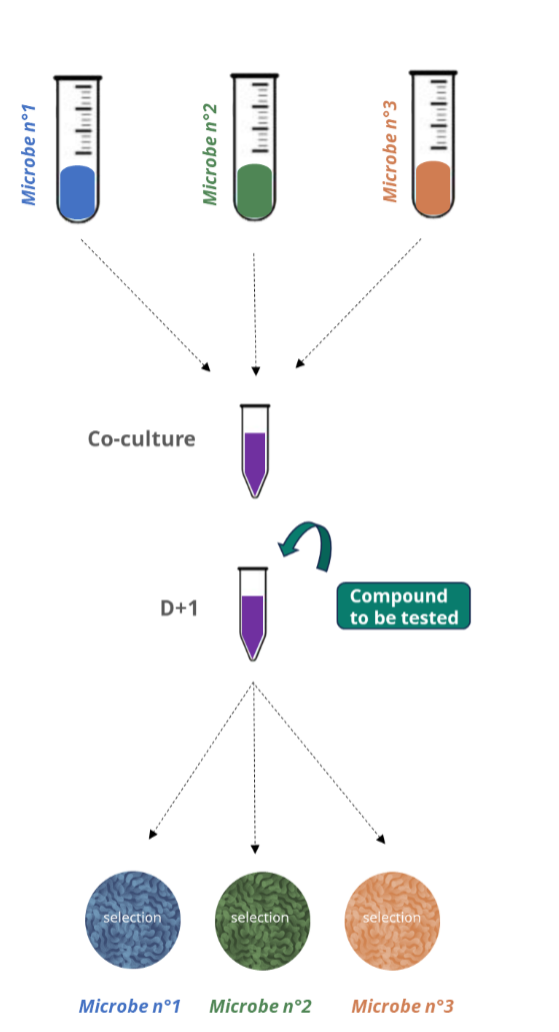
Since Malassezia fungi cannot produce their own fats, they secrete lipases to break down scalp's natural oils into essential nutrients for their survival. This process releases irritating by-products, specifically oleic acid, which penetrates and weakens the skin's protective barrier. This chemical irritation triggers an inflammatory response, leading to the rapid skin cell turnover and redness characteristic of both dandruff and seborrheic dermatitis.
Because lipases are essential for Malassezia survival and are the direct cause of the irritating by-products, they are a primary target for treatments.
Vibiosphen offers an in vitro lipase activity measurement using the 4-methyl umbelliferyl oleate (MUO) assay, that can be used to evaluate molecules in development.
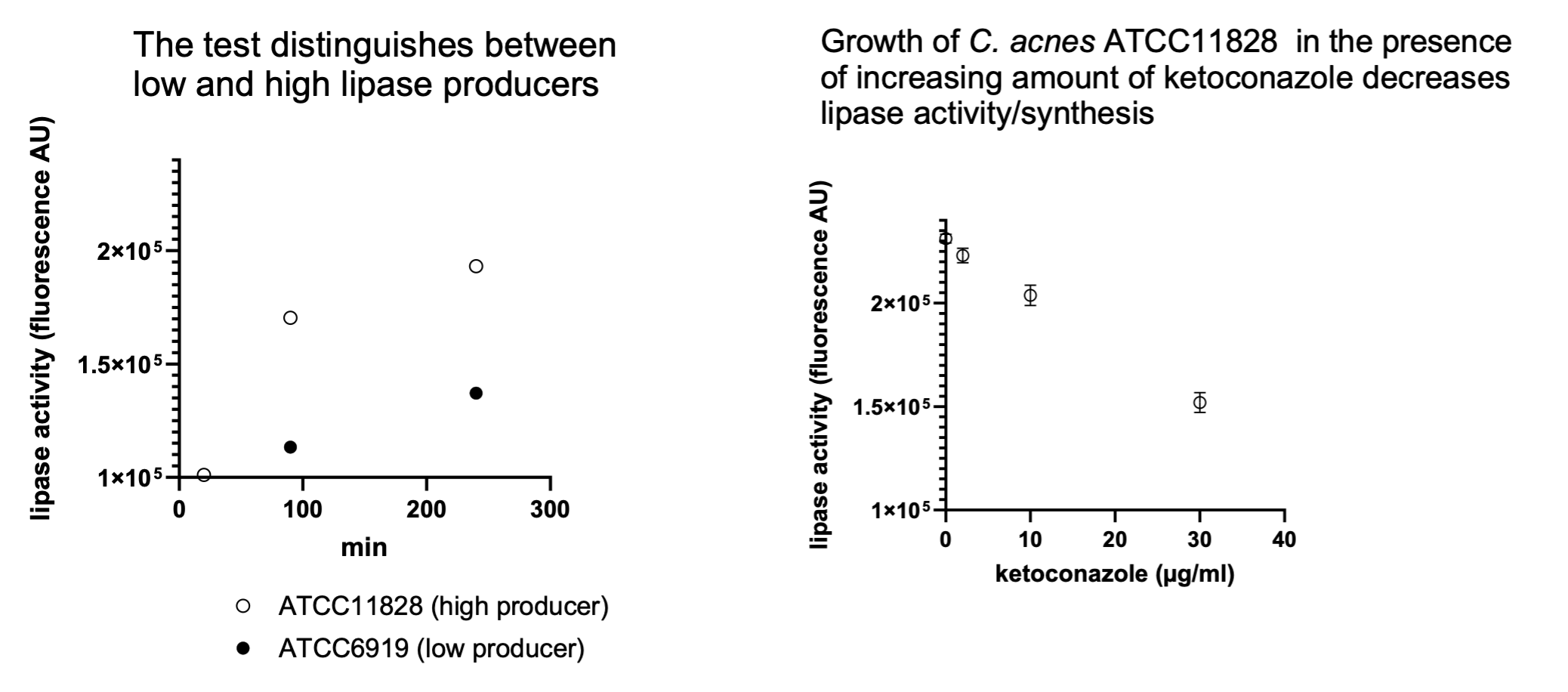
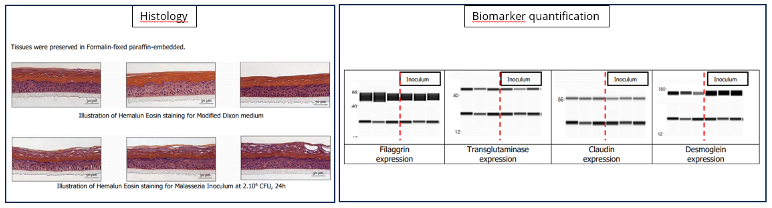
Seborrheic dermatitis and dandruff are characterized by a structurally disorganized stratum corneum featuring immature skin cells and a significant deficiency in long-chain ceramides. This weakened barrier allows pro-inflammatory fungal metabolites (specifically oleic acid from Malassezia) to penetrate the skin, triggering a cycle of irritation and rapid cell turnover.
Vibiosphen has developed 3D models where human skin explants or reconstructed human epidermis (RHE) are colonized by the microbial species of interest.
The exact mechanisms of how the gut microbiota is linked to the onset and development of Seborrheic dermatitis and dandruff have not been fully established. By analogy with other immune-based inflammatory diseases such as atopic dermatitis, psoriasis, or acne vulgaris and with evidence of the existence of the gut–skin axis, it is likely that the main mechanism participates in the inflammatory immune response.
